In recent weeks, at least three incidents of botulism contamination of three different foods have caused recalls in Europe.
- Contaminated broccoli was linked to the death of one man and hospitalization of nine others in Italy. The broccoli was in a sandwich purchased from a street-food van.
- Contaminated guacamole from a traveling festival in Italy has been linked to the death of one woman and illness of at least six.
- Jarred carrots used in a carrot cake has been linked to the death of one woman and the hospitalization of six others who shared a meal that included the cake.
Botulism is a rare but serious illness caused by the toxins produced by Clostridium botulinum bacteria which attacks the body’s nerves and causes difficulty breathing, muscle paralysis, and even death. It is the spores of the bacteria that, under certain conditions (such as low acid, sugar, salt, or oxygen at high temperatures), can grow and make one of the most lethal toxins known. One example, which likely led to at least some of the European cases is that of improperly home-canned, preserved, or fermented foods. When people eat these foods, they can become seriously ill, or even die, if they don’t get proper medical treatment quickly.
However, the only specific treatment for non-infant botulism is the Botulism Antitoxin Heptavalent (BAT), which contains antibodies against all seven known botulinum toxin types (A-G). But it is not routinely stocked at hospitals due to its rarity of use, relatively short expiration date, and specialized storage requirements. Rather BAT is available only from CDC through a specific system. To attain the antitoxin, which is stored at CDC Port Health Stations in major airports around the nation, clinicians have to contact their state health department’s 24-hour telephone number. The state health department will then contact the CDC for a clinical consultation and, if indicated, will facilitate the emergency release of the antitoxin. Other countries have similar restrictions and systems for attainment of the antitoxin.
It is important to note that infant botulism is different in both the illness and treatment. While still resulting from the swallowing of botulism bacteria, it is an intestinal toxemia in which the spores temporarily colonize an infant’s large intestine and produce botulinum neurotoxin. It is treated with the Botulism Immune Globulin Intravenous (Human) (BIG-IV) “BabyBIG,” which can only be procured by a treating physician from the California Department of Public Health Infant Botulism Treatment and Prevention Program (IBTPP)
Foodborne infant botulism is most often associated with honey, but as recently reported, a 2024 case was caused by the feeding of peanut butter to a six-month-old, which had not previously been seen as a vehicle for infant botulism.
COVID Risk Matrix:
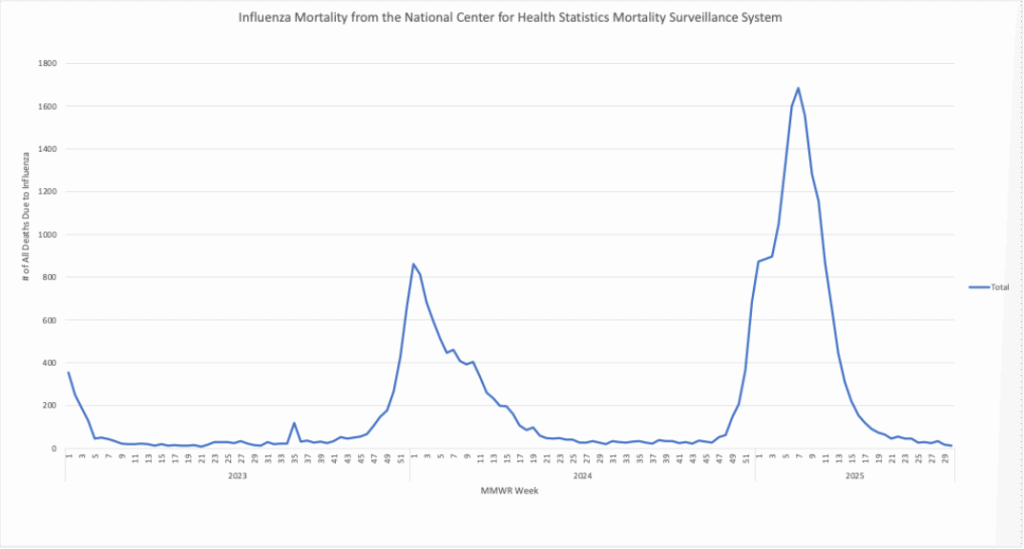
Influenza:
Public Health News:
- From 2009–2021, the CDC’s Animal Contact Outbreak Surveillance System (ACOSS) recorded 557 U.S. outbreaks of enteric illnesses linked to animal contact, causing 14,377 illnesses, 2,656 hospitalizations, and 22 deaths. Salmonella was the leading cause, most often tied to poultry—especially backyard flocks—followed by Cryptosporidium from ruminants and Salmonella from turtles. While multistate outbreaks made up less than one-third of reported events, they accounted for the majority of cases, hospitalizations, and deaths. Most exposures occurred in private homes, highlighting gaps in hygiene and disease-prevention knowledge among animal owners. The report stresses the importance of continued surveillance, public health education, and a coordinated One Health approach to reduce these illnesses.
- HHS Secretary Robert F. Kennedy Jr. has ended all federal mRNA vaccine development, canceling $500 million in contracts, including an H5N1 project. Experts warn the decision will set vaccine science back a decade, weaken pandemic preparedness, and cost lives, as mRNA technology enables much faster production than the outdated whole-virus approach Kennedy favors.
- A study of over 140,000 U.S. children under 5 found that recent COVID-19 infection did not increase the risk of contracting RSV, unlike influenza, which was linked to higher RSV odds. Researchers concluded that SARS-CoV-2 does not appear to suppress immunity in a way that raises RSV risk.
- Cambodia reported its 15th human case of H5N1 avian flu this year: a 6-year-old girl from Takeo province hospitalized with fever, cough, and breathing difficulties. Investigations found nearly 1,000 sick or dead chickens in her village and home, with her mother recently handling some dead birds. Cambodia has a high fatality rate from H5N1, with 7 of 15 cases this year fatal and an overall case-fatality rate of 57.5% since 2005. Most recent infections involve contact with sick poultry and a new virus reassortant circulating since late 2023, with cases rising sharply this summer.
- An outbreak of Legionnaires’ disease in Harlem has resulted in 83 confirmed cases and three deaths since late July. City health officials link the outbreak to contaminated cooling towers, which have been treated to stop the spread of Legionella bacteria. Eleven towers testing positive have been remediated, but the city has not disclosed the specific affected buildings, citing medical privacy concerns. Officials urge residents with flu-like symptoms to seek medical care.




